A review of the development of the Collaborative Family Health Nursing Project in Europe
Sección: Enfermería familiar y comunitaria en el ámbito internacional
Cómo citar este artículo
Duffy T, Johnston B, Martin P, Martínez Riera JR, Giménez Maroto A, Atkinson J, et al. A review of the development of the Collaborative Family Health Nursing Project in Europe. RIdEC 2011; 4(2):52-5.
Autores
1Tim Duffy, 2Brian Johnston, 3Paul Martin, 4José Ramón Martínez Riera, 5Ana Giménez Maroto, 6John Atkinson, 7Pauline Banks,
Contacto:
Email: Tim.Duffy@uws.ac.uk
Titulo:
A review of the development of the Collaborative Family Health Nursing Project in Europe
In general terms, the population of the world is becoming healthier and consequently living longer. Despite such positive progress, there continue to be many global health challenges. For example, over 7 million people have High Blood Pressure which contributes to 13% of deaths. The volume of people diagnosed with diabetes is likely to double by the year 2030, the lack of physical activity is expected to contribute to 6% of deaths while overweight and obesity may contribute to a further 5% of deaths (WHO, 2009a).
The above noted risks are recognised as key contributors to a range of chronic diseases including heart disease and cancers and these are evident across all income groups in all countries (WHO, 2009a). Further areas of significant health concern across the globe include childhood obesity, Mental Health, HIV and alcohol and drug disorders.
The United Nations set out the Millennium Development Goals and these include the eradication of extreme poverty and hunger; the achievement of universal primary education; the promotion of gender equality and empowerment of women; the reduction of child mortality; the improvement of material health; the combating of HIV/AIDS, malaria and other diseases; the drive towards environmental sustainability and global partnership for development (WHO, 2010).
Healthcare personnel throughout the world are crucial in meeting such global needs and many countries lack appropriate numbers of physicians, nurses and midwives to adequately meet the primary care demands noted by the Millennium Development Goals (WHO, 2010). In order to address these Goals, many countries must review and improve the way they train, deploy, support and monitor their healthcare workforce. Clearly such a process has considerable financial implications and it is relevant to note that the Commission on Social Determinants of Health (2008) recognises that staff such as community health workers can provide low cost healthcare provision. Within Europe the role of the Family Health Nurse (FHN) has been recognised as a generalised one which can make available support in the family home. Such support can assist achieve the HEALTH21 aims by “promoting and protecting people’s health throughout the course of their lives; and reducing the incidence of and suffering from the main diseases and injuries” (WHO, 1998).
Specifically, for the nursing and midwifery profession the WHO (2010) has provided a common goal within a vision statement for nursing and midwifery service. The common goal is to seek “Improved health outcomes for individuals, families and communities through the provision of competent, culturally sensitive, evidence-based nursing and midwifery services” (WHO, 2010).
WHO (2010) highlights the importance of the nursing and midwifery profession in the delivery of quality health services. Furthermore, to sustain future capacity and maximising the full potential of this valuable resource there requires to be ongoing investment in nursing and midwifery in areas including service improvement, deployment and education to this professional group.
Within the context of Europe the WHO (2011) provided a vision for health and well-being within the region: “Our vision is for a WHO European Region in which all people are enabled and supported in achieving their full health potential and well-being and in which countries, individually and jointly, work towards reducing inequities in health within the Region and beyond” (WHO, 2011).
Guidance towards the development of the Family Health Nurse was provided by the World Health Organisation in 2000 when the document The Family health Nurse: Context, conceptual Framework and Definitive Curriculum was published. A variety of roles were expected of the Family Health Nurse care provider and consequently such staff would require a wide range of skills including those of decision making, communication, leadership and management. It was anticipated that they would provide early intervention, a range of treatment options, advice, signposting of services, public health care and social support (WHO, 2000a).
Following the WHO guidance in 2000, various European countries have embarked on the development of the role of the Family Health Nurse. Progress has been significant while varied in for example Tajikstan, Kyrgzstan, Moldova, Scotland and Germany (Hennessy and Gladin, 2006). Parfitt and Cornish (2007) amongst others note the positive contributions that have been made by Family Health Nurses in relation to preventive health. Results from a Scottish study (Murray, 2008) identified three key findings. Firstly that the Family Health Nurse is particularly useful in remote, rural or sparsely populated areas; secondly that rollout of the Family Health Nurse initiative is likely to be problematic if a ‘takeover’ or ‘replacement’ model is put in place; and thirdly that European agreement should be sought on the range of practice and training requirements of a Family Health Nurse with a view to the establishment of a pan-European Masters-level programme or equivalent cualfiication programme.
The European Family Health Nursing Collaborative Project
To build on the increasing knowledge and experience of developments of the Family Health Nursing role in Europe, a project team has been set up at the University of the West of Scotland. The team consists of the Vice Principal and Dean of Faculty of Education, Health and Social Sciences, three Professors, the Faculty Research and International Project Manager and a Masters by Research (MRes) student. This team, with the advice and guidance of WHO (Europe) personnel, has brought together Chief Nursing Officers, senior academic and research personnel from Armenia, Austria, Germany, Italy, Poland, Portugal, Romania, Scotland, Slovenia and Spain.
In January 2011 twenty six delegates from these countries met at a workshop in Berlin. This workshop was both a dynamic and successful event which focused on achieving mutual success of all collaborative partners.
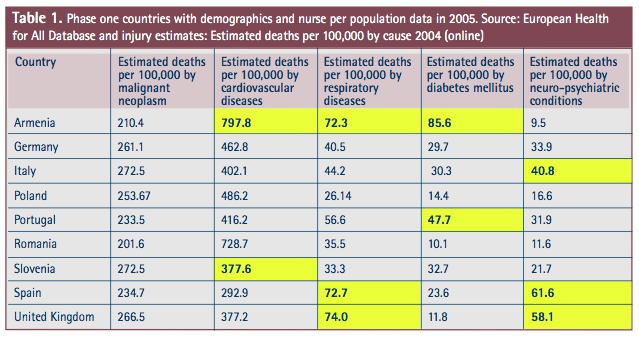
Data collated by the project team and presented at the workshop identified the key health problems within countries represented in the Family Health Nursing Project. This data can be seen in Table 1 below. There are clearly differences across countries in health related demographics. For example the estimated deaths per 100,000 by cardiovascular diseases is higher in Armenia and Romania and lowest in Spain, whereas estimated deaths per 100,000 by neuro-psychiatric conditions are higher in Spain and the United Kingdom and lowest in Armenia. Further difference can be observed across project partner countries in relation to respiratory diseases and diabetes mellitus. Such differences are important when planning the role of the healthcare workforce and in particular the role of the Family Health Nurse within each geographical and cultural context. The significance of these differences is even more concerning when the number of nurses per 100,000 available to deal with such health problems varies from 373 to 779 across phase one project partner countries.
The workshop also allowed evidence of differences between countries in the nursing education model for the role of FHN. In the case of Spain, according to the legislative framework in this country, the model for training specialists in Health Sciences (common to all health professionals) is being used, characterized by tutored self learning process in clinical units officially accredited for the multiprofessional training purpose, during the two years period of residence laid down in the postgraduate training programme.
Despite the differences in some key health related problems and training approaches, workshop delegates in Berlin agreed that there are a number of required outcomes for the future of the Family Healthy Nursing project including the development of a:
- Common pathway to Family Health Nursing.
- Collective descriptor of drivers for future change.
- Common vision of the purpose and focus of nursing in the community.
- Common understanding of capability pathways.
- Research focus on a multi country basis on impact and effectiveness of nursing in the community.
- Network of exchange and support in a ‘learning environment’ to support delivery of the vision.
- Strategy to enhance the status of nursing.
The use of online networks is an emerging method of connecting international organisations, as it considered both viable and cost effective (Sanderson, Gordon & Ben-Ari, 2008). The UWS project team are eager to use all appropriate methods to ensure effective communication and partner engagement.
Currently, the collaborative partners are engaged in facilitated online discussions on the following themes:
- Definition of Family Health Nursing and review of current practice across partner countries.
- Competency and capability requirements for Family Health Nurses working in communities including establishment of inter-country consensus on professional qualification level.
- The available education/training in partner countries.
- The available module materials suitable for delivery at undergraduate and postgraduate levels in a range of European languages.
- Identification of the evaluation framework including a minimum data set (e.g. key demographic drivers, health challenges).
To facilitate further development of this project, a number of funding applications have been prepared. One application for funding is to the European Commission Lifelong learning Programme within the Erasmus sub-programme.
Specific objectives of the Erasmus application are:
- To develop a definition for Family Health Nursing based on a systematic review of FHN and current practice across partner countries.
- To clarify competency and capability requirements for Family Health Nursing working in communities including establishment of inter-country consensus on professional qualification level.
- To review available education/training in partner countries.
- To develop module materials suitable for delivery at undergraduate and postgraduate levels in a range of European languages.
- To develop an evaluation framework including a minimum data set (e.g. key demographic drivers, health challenges).
Specific outcomes of the Erasmus application are expected to be:
- A shared understanding of the role of the Family Health Nursing incorporating required competencies, capabilities and training needs.
- Development of module materials suitable for delivery in partner countries.
- Identification of an appropriate baseline minimum dataset to facilitate evaluation (UWS Erasmus application, February 2011).
To date the Family Health Nursing project has focussed on and been driven by partners within Europe. This has enabled the project team to manage the project in a way that is advantageous to each collaborative partner. However, as the project has gained momentum, team members have been invited to present at a range of international nursing conferences. This has resulted in significant interest in this project from senior professional nursing and academic staff from the United States of America, Australia, Africa, Thailand, Ireland and Mongolia. The project team members are keen that the key building blocks noted above in this paper are put in place before wider geographical participation and dissemination is embarked on with these countries.
Conclusion
The World Health Organisation has strongly advocated the concept of Family Health Nursing. For a number of years, various European countries have developed considerable experience in developing and delivering the approach including designing and delivering appropriate training programmes. Research literature supports the importance of the Family Health Nursing role development and there are major health and cost related advantages in deploying this healthcare role in appropriate and targeted communities across Europe.
The project team based at the University of the West of Scotland has brought together key personnel from ten European countries to share evidence and experience with a view to developing appropriate atrainig and practice based programmes for Family Health Nurses. The intention is that as a collaborative partnership, a consistent approach will be adopted which not only has high standards of quality but also takes into consideration, promotes and values contextual requirements. Further international development of this project will be facilitated in the near future to include countries out-with Europe.
References
- Commission on Social Determinants of Health. Closing the gap in a generation: health equity through action on the social determinants of health. Final report of the Commission on Social Determinants of Health. Geneva: World Health Organization; 2008.
- Hennessy D, Gladin L. Report on the evaluation of WHO multi-country family health nurse pilot study. Copenhagen: WHO regional Office for Europe; 2006.
- Murray I. Family Health Nurse Project-An Education Program of the World Health Organization. Journal of Family Nursing 2008; 14(4):469-485.
- Parfitt B, Cornish F. Implementing Family Health Nursing in Tajikistan: From policy to practice in primary health care reform. Social Science & Medicine 2007; 65:1720-29.
- Sanderson T, Gordon D, Ben-Ari G. International Collaborative Online Networks: Lessons Identified from the Public, Private, and Non-profit Sectors. Washington DC: Center for Strategic & International Studies; 2008. [Online] Available: http://csis.org/files/media/csis /pubs/081211_sanderson_intlcollab_web.pdf
- World Health Organisation, Regional Office for Europe. Health21 an introduction to the health for all policy framework for the WHO Europe, 1998. [Online]. Available: http://www.euro.who.int/__data/assets/pdf_file/0003/88590/EHFA5-E.pdf
- World Health Organisation, Regional Office for Europe. Munich Declaration: Nurses and midwives: A force for health. Geneve: WHO Europe; 2000(a). [Online]. Available: http://www.euro.who.int/eprise/main/who/aboutwho/policy/20010828_4
- World Health Organization. The Tallinn Charter: Health Systems Health and Wealth. Copenhagen: World Health Organization; 2008. [Online]. Available: http://www.euro.who.int/__data/assets/pdf_file/ 0008/88613/E91438.pdf
- World Health Organization. Global Health Risks: Mortality and burden of disease attributable to selected major risks. Geneva: World Health Organization; 2009(a). [Online]. Available: http://www. who.int/healthinfo/global_burden_disease/GlobalHealthRisks_report_full.pdf
- World Health Organization. European Health for All Database HFA-DB, 2010. [Online]. Available: http://data.euro.who.int/hfadb/
- World Health Organization. Millennium Development Goals in the WHO European Region. Copenhagen: World Health Organization; 2010 [Online]. Available: http://www.euro.who.int/__data/assets/pdf_file/ 0003/87438/E93723.pdf
- European Region: A situational analysis at the eve of the five-year countdown. Copenhagen: World Health Organization; 2010. [Online]. Available: http://www.euro.who.int/__data/assets/pdf_file/0003/ 87438/E93723.pdf
- World Health Organization. Nursing and Midwifery Services: Strategic Directions 2011-2015. Geneva: World Health Organization; 2010. [Online]. Available: http://whqlibdoc.who.int/hq/2010/ WHO_HRH_HPN_10.1_eng.pdf
- World Health Organization. Disease and injury estimates: Estimated deaths per 100,000 by cause 2004. [Online]. Available: http://www.who.int/healthinfo/global_burden_disease/estimates_country/en/index.html
- World Health Organization. A brief overview Health 2020: a new approach to health and well-being in Europe (2011). [Online]. Available: http://www.euro.who.int/__data/assets/pdf_file/0005/ 145688/HCP_Liege_2020_brief_overview.pdf

